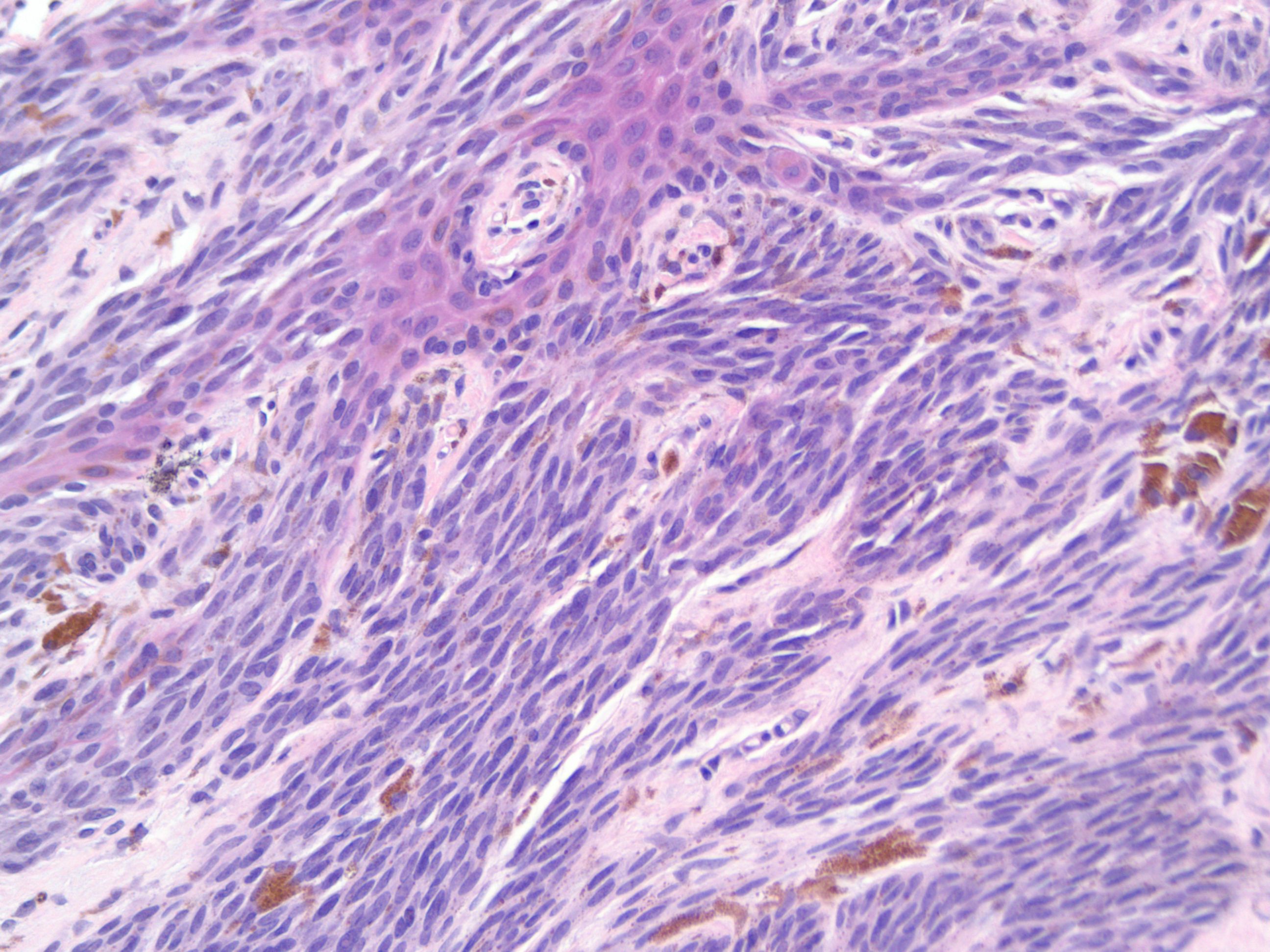 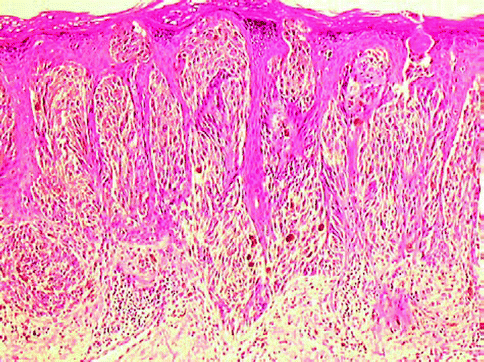
There appears to be a morphologic continuum between desmoplastic melanoma and vertical growth phase spindle cell melanoma, the latter being the most frequent type of invasive melanoma seen in lentigo maligna melanoma. Histologyĭesmoplastic melanoma is a form of vertical growth phase melanoma in which the invasive tumor cells have a spindled morphology and are associated with a striking desmoplastic stromal response ( Figures 1, 2, 3, 4, 5 and 6). 15 The probability of 5-year survival for tumors greater than 4 mm in thickness is higher than that for other types of melanomas that are of similar thickness, 6, 17 as alluded to above. 16 Neurotropism strongly enhances the statistical likelihood of local recurrence. 9 Local recurrences were noted in 29% of patients in one series of 58 desmoplastic and/or neurotropic melanomas, with a malignant cranial neuropathy occurring in four patients and death from metastatic disease in 19% of cases. In patients with multiple recurrences, invasion of adjacent structures such as salivary gland, periosteum, glenoid fossa, and cranial cavity can be seen. The lesions show a high recurrence rate, with recurrent tumors typically being amelanotic and presenting as an area of scarring or induration with palpable, ill-defined margins. Carlson et al, 6 who reported an equal distribution in men and women, found most tumors to be located in the head and neck area (75%) and to be nonpigmented (57%) they concluded that most desmoplastic melanomas took origin in neoplasms that were of lentigo maligna subtype. The classical clinical finding is that of a pale or fleshy firm nodule reminiscent of a scar, which tends to delay clinical diagnosis and biopsy. 15 Although any given desmoplastic melanoma can be deeply invasive, when matched for depth of invasion, they are associated with a lesser risk of metastatic disease than conventional melanomas of similar depth. Typically, they occur in older patients, with mean ages in the larger series falling into the sixth to eighth decades of life. 3 Desmoplastic melanomas tend to occur in the head and neck area and the upper back 4, 5, 6, 7 but are also seen in mucosal sites such as the vulva or gingiva 8 and in acral locations. That said, only half of desmoplastic melanomas are clinically pigmented. 2, 3 The clinical clue to the diagnosis, when present, is cutaneous or mucosal pigmentation overlying a palpable dermal or submucosal nodule. Sometimes there is pronounced mucin deposition that imparts a boggy quality to the lesion. 1 Desmoplastic and neurotropic melanoma may be mistaken clinically for a scar, a fibroma, a basal cell carcinoma, or a fibromatosis. In this review, we will discuss in some detail certain of these novel clinicopathologic types of melanoma, as well as the abnormal phenotypic expressions seen in vertical growth phase melanoma.ĭemoplastic melanoma is a rare variant of malignant melanoma first recognized in 1971. Abnormal immunohistochemical expression of CD 34, cytokeratins, epithelial membrane antigen, and smooth muscle markers as well as the deficient expression of S100 protein and melanocyte lineage-specific markers such as GP100 protein (ie HMB-45 antibody) and A103 (ie Melan-A) also present confusing diagnostic challenges. Metaplastic change in melanoma, balloon cell melanoma, signet-ring cell melanoma, myxoid melanoma, small cell melanoma and rhabdoid melanoma all have the potential to mimic metastatic and primary neoplasms of different lineage derivations. Also problematic are the unusual phenotypic profiles seen in vertical growth phase melanomas these include those tumors whose morphological peculiarities mimic cancers of nonmelanocytic lineage and those melanomas that express aberrant antigenic profiles not commonly associated with a melanocytic histogenesis. Of these, the more treacherous examples include the desmoplastic melanoma, the nevoid melanoma, the so-called ‘minimal-deviation melanoma,’ melanoma with prominent pigment synthesis or ‘animal-type melanoma,’ and the malignant blue nevus. A potential diagnostic pitfall in the histologic assessment of melanoma is the inability to recognize unusual melanoma variants.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
